3 things you need to know about TMJ pain
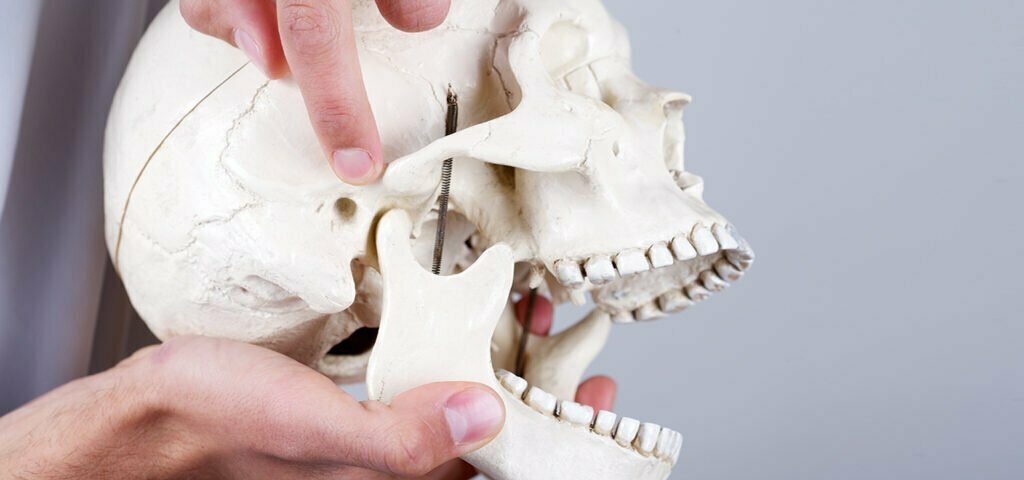

The temporomandibular joint (TMJ), is formed by your skull and jawbone. It acts like a sliding hinge and is responsible for opening and closing your mouth, enabling you to talk, chew, and yawn.1,2
TMJ pain can be debilitating – just ask Dr. Sasha Hamid, a chiropractor in Ottawa, Ontario. When she was in middle school, she started experiencing severe headaches. Her jaw would get stuck in place and sometimes dislocate. The pain was so severe that she could not concentrate at school and was unable to participate in extracurricular activities.
Sasha was born with a small jaw and needed surgery to relieve her pain, but she could not have it until she was off the pain medications that were getting her through the day for six months. Unsure how she would manage this pain without medication, her surgeon referred her to a chiropractor.
“My chiropractor was the first person to explain why this was happening in a way that I understood,” says Dr. Hamid. “He gave me exercises and put me in control of managing my pain. Thanks to him, I was completely off any pain medications within six months and was able to manage the symptoms through acupuncture, stretches, and manual techniques.”
This experience was what inspired Dr. Hamid to become a chiropractor.
The causes of TMJ pain
The bones of the TMJ are separated by a disc of cartilage to keep your jaw moving smoothly.3 When those muscles become irritated, the disc is displaced. Common symptoms include popping, a clicking sound or sensation, muscle tenderness, joint tenderness, and being unable to open your jaw wide.4
There are three main categories of TMJ pain:
- The most common is in the muscles that control the jaw and the connecting neck and shoulder muscles;
- Internal disorder of the joint, or a dislocated or displaced disc; and
- A degenerative joint disease in the jaw joint, like arthritis.5
Your risk of developing this pain is increased by jaw injury, stress, or grinding and clenching your teeth.3
Managing TMJ pain
There are several things you can do to treat or reverse TMJ-related pain:
- Eating softer foods
- Applying ice packs
- Avoiding extreme jaw movements
- Learning techniques to relax and reduce stress
- Practicing gentle stretching of the jaw to help increase its movement2
- Soft tissue massage
Chiropractors can help
Chiropractors can help in a number of ways, including:
- Joint manipulation to help restore movement
- Nearby muscle release by going through the mouth
Talk to your chiropractor about a treatment that is right for you.
REFERENCES:
1. Yuill E, Howitt S. Temporomandibular joint: conservative care of TMJ dysfunction in a competitive swimmer. J Can Chiropr Assoc. 2009;53(3): 165-72.
2. TMJ Disorders. National Institute of Health website. https://www.nidcr.nih.gov/oralhealth/Topics/TMJ/TMJDisorders.htm. Published April 2015. Accessed February 14, 2017.
3. TMJ disorders: Overview. Mayo Clinic website. https://www.mayoclinic.org/diseases-conditions/tmj/home/ovc-20209398. Accessed February 1, 2017.
4. George JW, Fennema J, Maddox A, Nessler M, Skaggs CD. The effect of cervical spine manual therapy on normal mouth opening in asymptomatic subjects. J Chiropr Med. 2007; 6(4): 141-5. doi: https://dx.doi.org/10.1016/j.jcme.2007.08.001.
5. Vinjamury SP, Singh BB, Khorsan R, Comberiati R, Meier M, Holm S. Chiropractic treatment of temporomandibular disorders. Altern Ther Health Med. 2008; 14(4): 60-3.
6. Brantingham JW, Cassa TK, Bonnefin D, et al. Manipulative and multimodal therapy for upper extremity and temporomandibular disorders: A systematic review. J Manipulative Physiol Ther. 2013; 36(3): 143-201. doi: 10.1016/j.jmpt.2013.04.001.
7. Randhawa K, Bohay R, Côté P, et al. The effectiveness of noninvasive interventions for temporomandibular disorders: A systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Clin J Pain. 2016; 32(3): 260-78. doi: 10.1097/AJP.0000000000000247.